Patrick Cherfan, Efthymios D Avgerinos, Rabih A Chaer
|
Abstract Nutcracker syndrome refers to the symptomatic extrinsic compression of the left renal vein presenting most commonly as flank pain and haematuria. While surgery remains the first-line treatment, stenting is gaining more acceptance and there are now several published case series. This article highlights the outcomes of left renal vein stenting in the setting of nutcracker syndrome. Disclosure: The authors have no conflicts of interest to declare. Received: Accepted: Published online: Correspondence Details: Rabih A Chaer, Room 351.4, Division of Vascular Surgery, University of Pittsburgh Medical Center, 200 Lothrop St, South Tower, Pittsburgh, PA 15213–2582, US. E: chaerra@upmc.edu Open Access: This work is open access under the CC-BY-NC 4.0 License which allows users to copy, redistribute and make derivative works for non-commercial purposes, provided the original work is cited correctly. |
First described in 1937, the classic nutcracker syndrome (NCS) refers to the entrapment of the left renal vein (LRV) between the superior mesenteric artery (SMA) and the aorta.1 While the mainstay of treatment remains surgery, which is supported by good long-term outcomes, LRV stenting is an emerging alternative to open repair.2 The first successful case of LRV stenting was described by Neste et al. in 1996, and was performed in a patient who had a history of pancreatic cancer treated with a Whipple procedure, chemotherapy and radiation.3
Although patients with NCS are typically young and healthy, avoiding laparotomy and its associated complications makes stenting appealing, especially in patients with recurrent stenosis following renal vein transposition.4 With much of the natural course of this disease being unknown with no established prevalence, case series are a valuable addition to the relatively sparse published evidence for the procedure.5,6 The purpose of this article is to highlight the outcomes of LRV stenting as described in recent case series.
Overview
LRV stenosis or NCS can have variable clinical presentations, with haematuria and flank pain being by far the most common presenting symptoms.7,8 A recent systematic review pointed towards an agreement among several investigators that an SMA branching angle of <35° is required in order to establish a diagnosis.9 However, the gold standard for diagnosis remains venography with a renocaval pullback pressure gradient of ≥3 mmHg.7 There is a subset of patients who have incidental findings of NCS or LRV stenosis on duplex/CT imaging; however, these people do not need intervention in the absence of clinical symptoms.10
Treatment should be tailored to the individual patient but non-surgical treatment should be attempted first for at least 6 months in all cases. In patients younger than 18 years, spontaneous remission is very common due to anatomic factors related to development and the distribution of body fat.7,11 Angiotensin-converting enzyme inhibitors and aspirin have also been used to improve orthostatic proteinuria and renal perfusion.12,13 Correction will be needed not only to ease persistent debilitating symptoms, but also to protect against possible complications, such as renal vein thrombosis, chronic glomerulopathy and compromised kidney function.8,14,15
Surgical Treatment
Surgery remains the gold standard modality. A retrospective review of data from 36 patients who underwent several types of open surgery at the Mayo Clinic in the US demonstrated an overall resolution of symptoms exceeding 80%.2 The most commonly studied and performed surgery is LRV transposition. This is followed by gonadocaval bypass, SMA transposition, kidney auto transplantation and fibrous tissue resection at the aortomesenteric angle. Other much less commonly performed procedures are nephropexy, laparoscopic splenorenal venous bypass and external stenting of the LRV with a ringed polytetrafluoroethylene (PTFE) graft.7,16–18 However, surgery is not without complications and recurrent haematuria, LRV thrombosis and retroperitoneal haematoma have all been observed.16,19
Endovascular Treatment
Endovascular treatment of LRV stenosis has gained favour since its introduction in 1996, due to the ease of the procedure compared to open surgery, and its lower morbidity secondary to its minimally invasive nature. This procedure can often be done under local anaesthesia and sedation. Despite its minimal invasiveness, LRV stenting lacks robust evidence mainly regarding its durability. For this reason, as with any other intervention, the decision to undergo stenting must be preceded by a thorough discussion with the patient about the risks, benefits and unknowns of LRV stenting. It is important to stress the fact that these procedures should be performed on symptomatic patients only and by experienced clinicians in endovascular suites that have fixed imaging capability.5 Failures and complications, such as stent migration, can be frequent and can be accompanied by serious sequelae, especially if certain procedural rules are not followed.
CT Scan Showing Compression of the Left Renal Vein
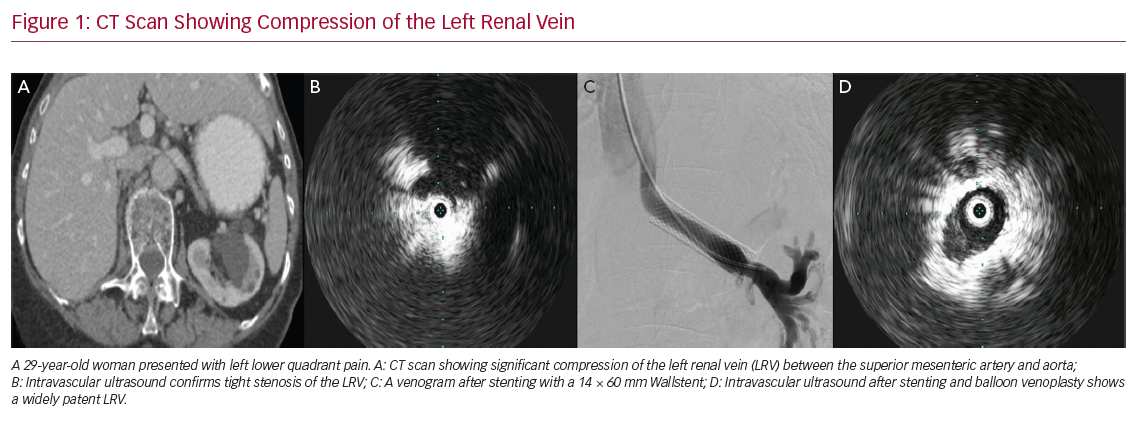
There are no great differences in terms of technique among different institutions. In most procedures, the LRV is accessed through the right common femoral vein, with some physicians preferring to use the left common femoral vein or even the right internal jugular vein. While access site is determined by the physician’s preference, there is no reported difference in terms of complications.7,20,21 After selective catheterisation of the LRV, venography with the Valsalva manoeuvre should be performed to confirm the diagnosis. Intravascular ultrasound (IVUS) is also increasingly used to confirm a diagnosis through pullback imaging and to determine proper stent sizing.12 This has eliminated the need for the more traditional diagnostic pressure drop criterion of >3 mmHg across the stenotic lesion.
Balloon venoplasty has no role in treatment due to the persistent external compression that leads to recompression upon deflating the balloon. Large self-expanding 4–6 cm stents that are 14–16 mm in diameter are typically appropriate. Smaller diameters are not recommended due to reported cases of stent migration.22 The Wallstent (Boston Scientific) has been the stent used in the majority of cases, but novel dedicated venous stents are entering the market and may become more popular for this procedure.23
Complications of LRV stenting treatment include stent thrombosis, migration, deformity, erosion, risk of reintervention and risk of conversion to open repair.22,24,25 A retrospective study from China that included 75 patients demonstrated a migration rate of 6.7%. Migration sites included the vena cava, right ventricle, right atrium and the left side of the renal vein. The main reason behind that was inappropriate stent sizing.2,10,22,24–26 The risk of stent migration can be minimised by oversizing the stent diameter. While partial protrusion of the stent into the inferior vena cava did not seem to cause complications, distal landing beyond the first branch of the LRV had been suggested to reduce stent migration but this is not to be encouraged due to the long-term disruption of smaller branches by the continuous radial force of the stent.6,27
Experiences from the University of Pittsburgh Medical Center
The most recent large retrospective case series from the US was published by the University of Pittsburgh Medical Center featuring 18 patients (17 women; mean age 38.1 ± 16.9 years) who underwent endovascular treatment.5 It demonstrated fewer perioperative complications when compared to previously published series. Among the 18 patients underwent stenting of the LRV, five had previously undergone a LRV transposition and had recurrent symptoms (or no improvement) within 7 ± 4.9 months. Failure was defined as symptom recurrence or no improvement along with imaging evidence of severe renal vein stenosis.
The most common presenting symptoms were flank pain (n=15) and haematuria (n=10). Selective catheterisation of the LRV was performed through the right common femoral vein. Of the 18 patients, 13 (72.2%) noted improvement or resolution of symptoms at a follow-up of 41.4 ± 26.6 months. Of the five who did not have an improvement, three had previously undergone LRV bypass and two eventually needed renal autotransplantation. One of the remaining two women was later diagnosed with endometriosis, which can have a presentation similar to NCS. Haematuria resolved in 60%, which can be explained by the vascular changes resulting from chronic venous hypertension that cannot be reversed even with open surgery.5,16,19 Three underwent stent reintervention. The two-year primary and primary-assisted patency was 85.2% and 100% respectively.
No stent migration occurred, which highlights the importance of accurate stent sizing. This might have been influenced by the use of an IVUS in 61% of cases. Patients were started on dual antiplatelet therapy for 1–3 months and switched indefinitely to 81 mg aspirin.5 Figure 1 demonstrates the pre- and post-stenting imaging of a patient who underwent LRV stenting.
Other Published Literature
In a retrospective study including 61 patients in China with a median follow-up of 66 months, 59 patients noted improvement or resolution of symptoms within 6 months of LRV stenting. Postoperative complications included one stent migration to the hilar LRV, one stent migration into the right atrium, and one stent protrusion into the inferior vena cava. One perioperative complication of stent deployment in an LRV collateral was also reported.6
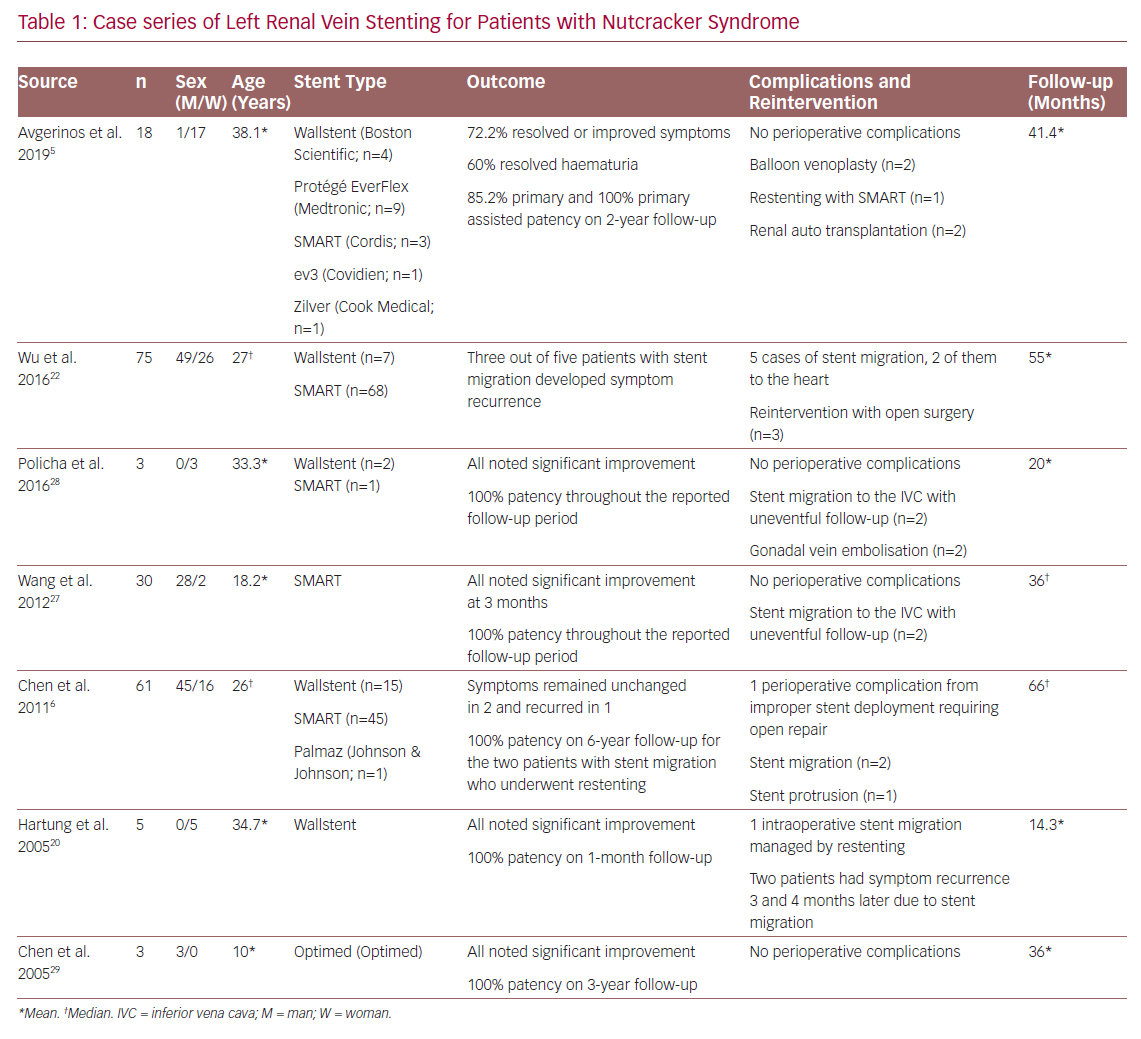
In another smaller Chinese case series, 30 patients underwent stenting of the LRV with a median follow-up of 36 months. Three months after stenting, complete resolution of haematuria and flank or abdominal pain was noted. No perioperative complications were recorded and two cases of stent prolapse into the inferior vena cava were found during routine follow-up at 12 months with no symptom recurrence or reintervention.27 Table 1 summarises the findings of the largest and most recent published series assessing outcomes of LRV stenting.
Case series of Left Renal Vein Stenting
LRV stenting is a safe and effective treatment modality for treating NCS that is refractory to conservative management. The most common reported complication is stent migration, and this risk could be eliminated with the accumulation of experience and expertise. LRV stenting should not be recommended as the gold standard as there is a lack of long-term data which would raise concerns about using the intervention in younger, otherwise healthy patients. The establishment of a registry is crucial to determine long-term outcomes of LRV stenting for patients with NCS.
- Grant J. A Method of Anatomy: Descriptive and Deductive. Baltimore, MD: Williams and Wilkins, 1944.
- Erben Y, Gloviczki P, Kalra M, et al. Treatment of nutcracker syndrome with open and endovascular interventions. J Vasc Surg Venous Lymphat Disord 2015;3:389–96.
Crossref| PubMed - Neste MG, Narasimham DL, Belcher KK. Endovascular stent placement as a treatment for renal venous hypertension. J Vasc Interv Radiol 1996;7:859–61.
Crossref| PubMed - Baril DT, Polanco P, Makaroun MS, et al. Endovascular management of recurrent stenosis following left renal vein transposition for the treatment of Nutcracker syndrome. J Vasc Surg 2011;53:1100–3.
Crossref| PubMed - Avgerinos ED, Saadeddin Z, Humar R, et al. Outcomes of left renal vein stenting in patients with nutcracker syndrome. J Vasc Surg Venous Lymphat Disord 2019;7:853–9.
Crossref| PubMed - Chen S, Zhang H, Shi H, et al. Endovascular stenting for treatment of Nutcracker syndrome: report of 61 cases with long-term followup. J Urol 2011;186:570–5.
Crossref| PubMed - Avgerinos ED, McEnaney R, Chaer RA. Surgical and endovascular interventions for nutcracker syndrome. Semin Vasc Surg 2013;26:170–7.
Crossref| PubMed - Berthelot JM, Douane F, Maugars Y, et al. Nutcracker syndrome: a rare cause of left flank pain that can also manifest as unexplained pelvic pain. Joint Bone Spine 2017;84:557–62.
Crossref| PubMed - Velasquez CA, Saeyeldin A, Zafar MA, et al. A systematic review on management of nutcracker syndrome. J Vasc Surg Venous Lymphat Disord 2018;6:271–8.
Crossref| PubMed - Quevedo HC, Arain SA, Abi Rafeh N. Systematic review of endovascular therapy for nutcracker syndrome and case presentation. Cardiovasc Revasc Med 2014;15:305–7.
Crossref| PubMed - de Macedo GL, Dos Santos MA, Sarris AB, et al. Diagnosis and treatment of the Nutcracker syndrome: a review of the last 10 years. J Vasc Bras 2018;17:220–8.
Crossref| PubMed - Ananthan K, Onida S, Davies AH. Nutcracker syndrome: an update on current diagnostic criteria and management guidelines. Eur J Vasc Endovasc Surg 2017;53:886–94.
Crossref| PubMed - Ha TS, Lee EJ. ACE inhibition can improve orthostatic proteinuria associated with nutcracker syndrome. Pediatr Nephrol 2006;21:1765–8.
Crossref| PubMed - Jin M, Hu P, Ding R, et al. Effectiveness of supine/standing urinalysis for differential diagnosis of left renal vein entrapment syndrome combined with or without glomerulopathy. Nephrology (Carlton) 2014;19:332–8.
Crossref| PubMed - Mallat F, Hmida W, Jaidane M, et al. Nutcracker syndrome complicated by left renal vein thrombosis. Case Rep Urol 2013;2013:168057.
Crossref| PubMed - Reed NR, Kalra M, Bower TC, et al. Left renal vein transposition for nutcracker syndrome. J Vasc Surg 2009;49:386–93; discussion 93–4.
Crossref| PubMed - Said SM, Gloviczki P, Kalra M, et al. Renal nutcracker syndrome: surgical options. Semin Vasc Surg 2013;26:35–42.
Crossref| PubMed - Yu S, Hu H, Ding G. Robot-assisted laparoscopic left renal vein transposition for the treatment of nutcracker syndrome: a preliminary experience. Ann Vasc Surg 2019;57:69–74.
Crossref| PubMed - Hohenfellner M, D’Elia G, Hampel C, et al. Transposition of the left renal vein for treatment of the nutcracker phenomenon: long-term follow-up. Urology 2002;59:354–7.
Crossref| PubMed - Hartung O, Grisoli D, Boufi M, et al. Endovascular stenting in the treatment of pelvic vein congestion caused by nutcracker syndrome: lessons learned from the first five cases. J Vasc Surg 2005;42:275–80.
Crossref| PubMed - Syed MI, Yu B, Akhter T, et al. Renal vein stenting via the right internal jugular approach with a provocative Valsalva maneuver to reduce the risk of stent migration. Perspect Vasc Surg Endovasc Ther 2011;23:268–71.
Crossref| PubMed - Wu Z, Zheng X, He Y, et al. Stent migration after endovascular stenting in patients with nutcracker syndrome. J Vasc Surg Venous Lymphat Disord 2016;4:193–9.
Crossref| PubMed - Rodriguez-Morata A, Robles-Martin ML, Reyes-Ortega JP. Endovascular treatment of posterior nutcracker syndrome with a new autoexpandable stent. J Vasc Surg Venous Lymphat Disord 2019;7:118–21.
Crossref| PubMed - Chen S, Zhang H, Tian L, et al. A stranger in the heart: LRV stent migration. Int Urol Nephrol 2009;41:427–30.
Crossref| PubMed - Rana MA, Oderich GS, Bjarnason H. Endovenous removal of dislodged left renal vein stent in a patient with nutcracker syndrome. Semin Vasc Surg 2013;26:43–7.
Crossref| PubMed - Chen Y, Mou Y, Cheng Y, et al. Late stent migration into the right ventricle in a patient with nutcracker syndrome. Ann Vasc Surg 2015;29:839e1–4.
Crossref| PubMed - Wang X, Zhang Y, Li C, et al. Results of endovascular treatment for patients with nutcracker syndrome. J Vasc Surg 2012;56:142–8.
Crossref| PubMed - Policha A, Lamparello P, Sadek M, et al. Endovascular treatment of nutcracker syndrome. Ann Vasc Surg 2016;36:295e1–7.
Crossref| PubMed - Chen W, Chu J, Yang JY, et al. Endovascular stent placement for the treatment of nutcracker phenomenon in three pediatric patients. J Vasc Interv Radiol 2005;16:1529–33.
Crossref| PubMed
